When I joined MCSP’s Haiti team to work on family planning (FP), we had an ambitious goal – to increase use of long-acting and permanent contraceptive methods in all 10 departments of the country. Given such methods were not readily accessible at the time, this was a tall order. But as a champion for women’s empowerment with a passion for FP, I was thrilled for the challenge.
With ardor, I developed strategies and, with colleagues, conducted several high-impact interventions:
- Introducing postpartum FP;
- Encouraging task-sharing to increase service delivery and increase access to FP methods;
- Establishing outreach through mobile clinics;
- Hosting more frequent sensitization campaigns on long-acting methods; and
- Strengthening service delivery sites.
After all of these efforts, I revisited the data and was stunned at what I found: no demonstrable change in one of the key indicators for assessing the impact of FP interventions – “couple years of protection,” commonly referred to as CYP. (USAID defines CYP as “the estimated protection provided by contraceptive methods during a one-year period, based upon the volume of all contraceptives sold or distributed free of charge to clients during that period.”)
How could this be?
An idea came to me. I crosschecked the data in stock reports about contraceptive commodities used against separate data on the users. These two reports – collected and analyzed by two different project partners – had considerable gaps. Moreover, I realized that a total of 83 institutions (almost half of the 164 facilities supported by the project) were missing data from two months or more in the system generating CYP. This omission and other errors (detailed in the chart below) began to clarify why we were calculating such low CYP.
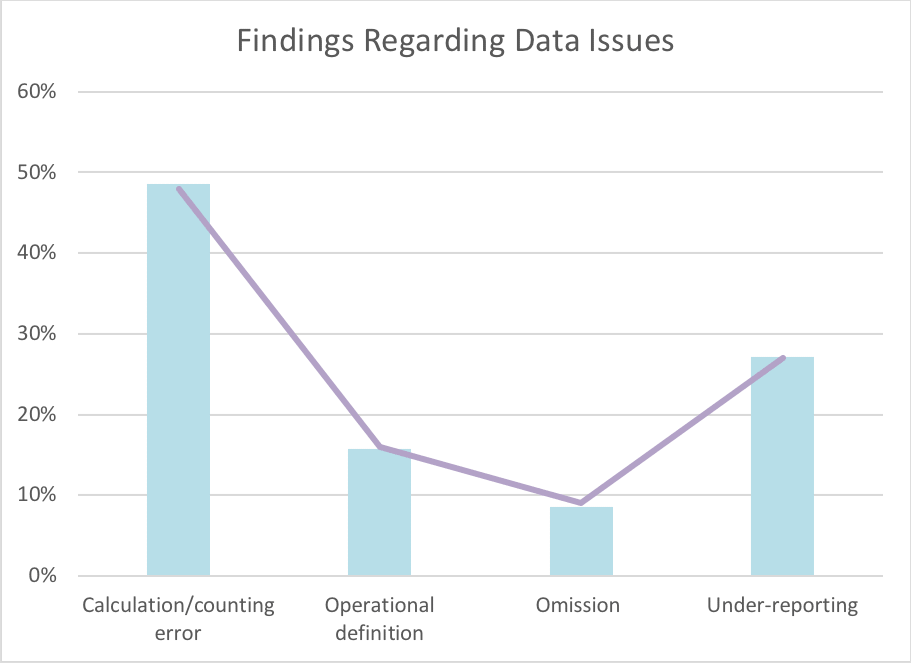
Disaggregation revealed errors in summing data (“calculation/counting error” above). Other times, a lack of understanding of the indicator confused users and acceptors (“operational definition” above). Methods offered were not reported, or there was no data at all in the system (“omission” above). There were also reports missing – for example, from the community level, within the health facility reports (“under-reporting” above).
My journey into the world of data was proving to be a bumpy one. Thankfully, all of these explanations accounted for the low CYP, which stood at 236,277 (or just 47% of the project’s annual target for October 2016-September 2017).
After these findings, I developed new corrective strategies and interventions in the management of family planning data:
- Making data management a decentralized and inclusive process, with data verification at each level of the health system – from the community to the health facility to the department;
- Strengthening the regional Ministry of Health bureaus on data quality control through regular support and training on data management (collection, chain of transmission, data entry, and interpretation); and
- Ensuring regular provision of reporting tools, systematic verification of data at the primary source level, and identification of weak points in the system.
After these interventions, the results were impressive:
- A total of 95% of institutions had complete and correct data;
- Data from the strengthened regions was regularly entered into the Ministry of Health’s unique reporting system on health statistics data across the country;
CYP for the same analysis period (Oct 2016-Mar 2017) increased from 236,277 (47% of the project’s annual target) to 313,110 (62% of the target) after the interventions. With several months to go, targets were ultimately met.
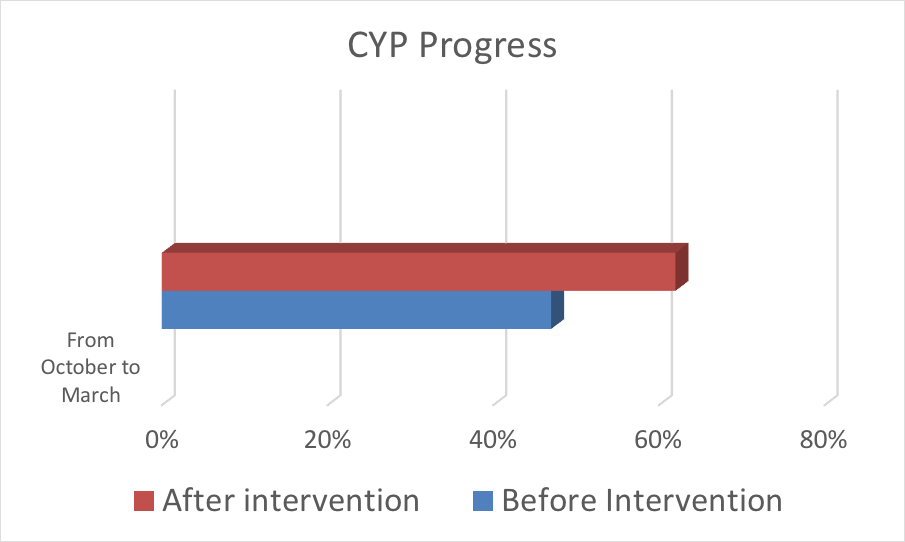
Adapting interventions to realities in the field allowed the project to achieve its objectives and reflect real results. To support the health system, supply chain and service delivery partners must routinely and efficiently coordinate well, including sharing data.
I learned a hard lesson: the reason for a gap between effort made and expected results may not be what you expect. You must get out of your comfort zone and expand your vision – and “think outside the box!”

